While living cells have been used for certain therapeutic applications for a long time, advanced engineered cell therapies have been shaping the headlines due to some spectacular successes in recent years. They hold great promise for treating cancer with commercial products to treat distinct cancers already in clinical use, and they represent emerging concepts to treat other conditions including, for example, inflammatory bowel disease, type-I diabetes, and refractory systemic lupus erythematosus. Moreover, they are in clinical trials to enhance the outcomes of solid organ transplantation.
(1) We visualize and quantify cell therapies after administration to living subjects.
This is important to better understand:
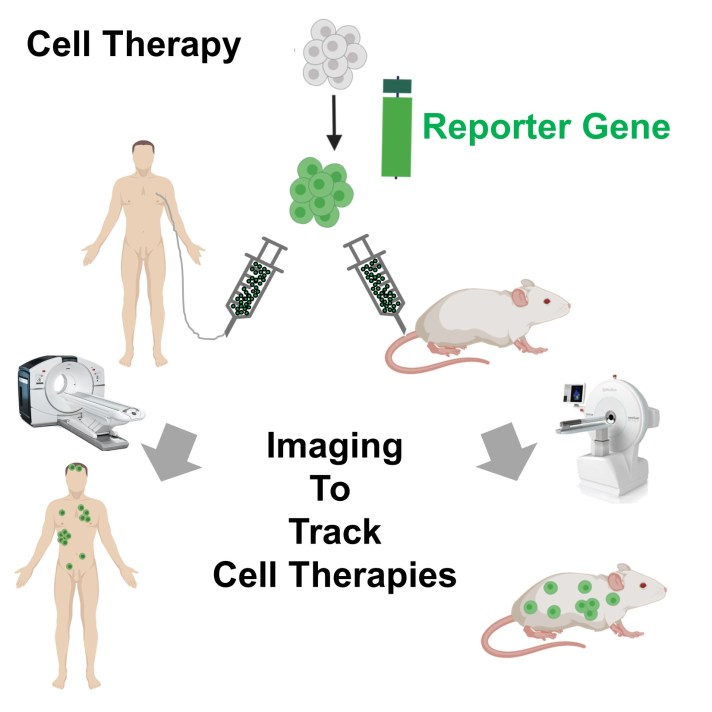
- where these live cell therapies localize to in the body,
- if they reach their intended target sites and whether they might also reach unintended tissues,
- how long they stay at the target tissues,
- if and to where they redistribute over time, and
- how long they survive within the body.
This knowledge is crucial for advanced cell therapy development and will help guide clinical use.
To achieve this, we develop non-invasive short and long-term in vivo cell therapy tracking approaches and apply them to various cell therapy settings in oncology and immunology.
| Chimeric antigen receptor T cell therapy (CAR-T) | Regulatory T cell therapy (regulatory T cells) | Stem cell-derived hepatocyte-like cells |
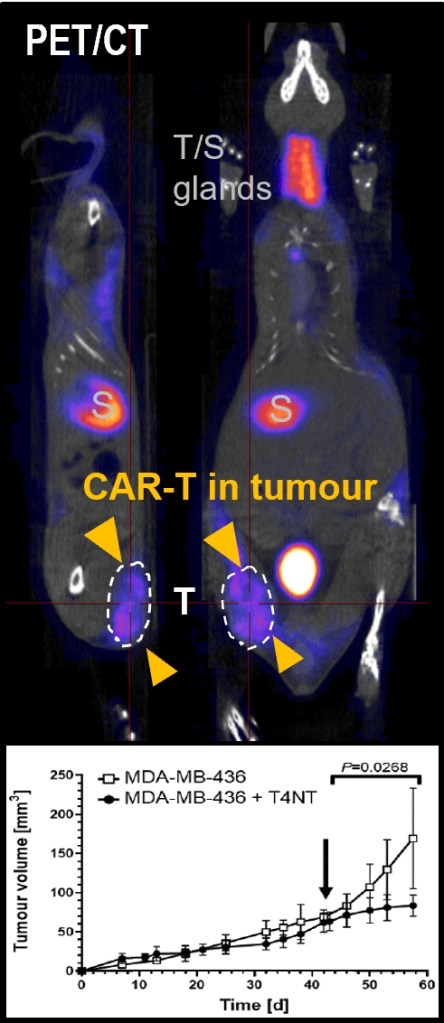
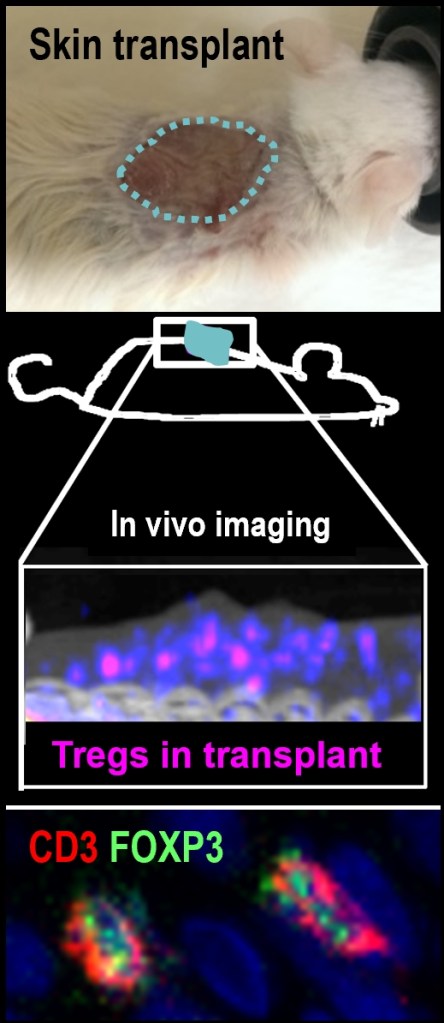
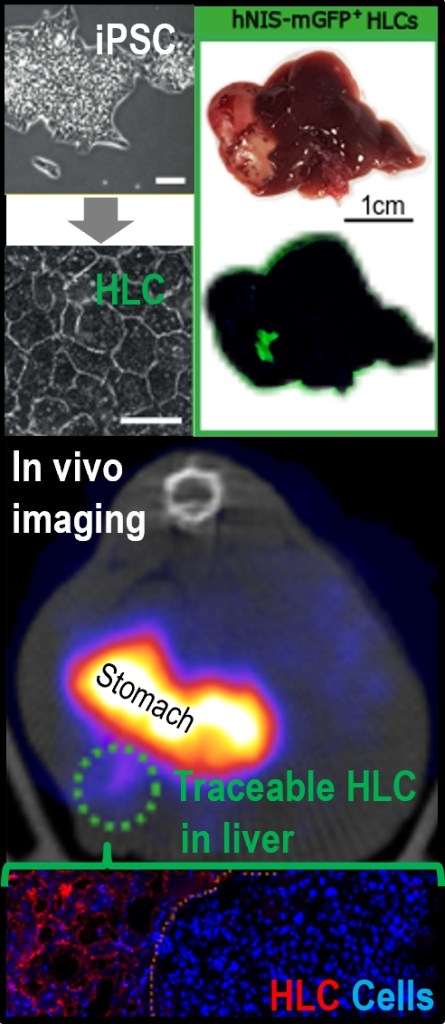
(2) We equip cell therapies with additional features to render them more powerful.
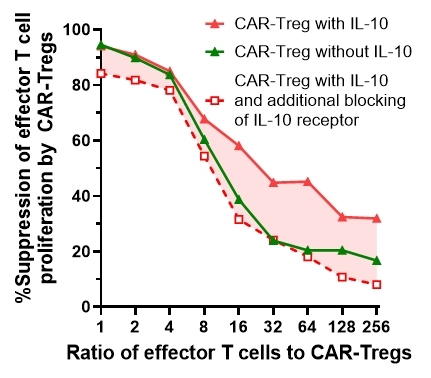
For example, we have succcessfully built the immunosuppressive cytokine IL-10 into CAR-Tregs. These IL-10 CAR-Tregs can alter their environment through secretion of this cytokine. IL-10 in the environment gives these CAR-Tregs an advantage in the quest to suppress the growth of nearby effector T cells.
In other projects, we develop CAR-T cells that turn on their additional features only when they are exposed to a specific environmental stimulus or when the antigen they are made to recognize is present.